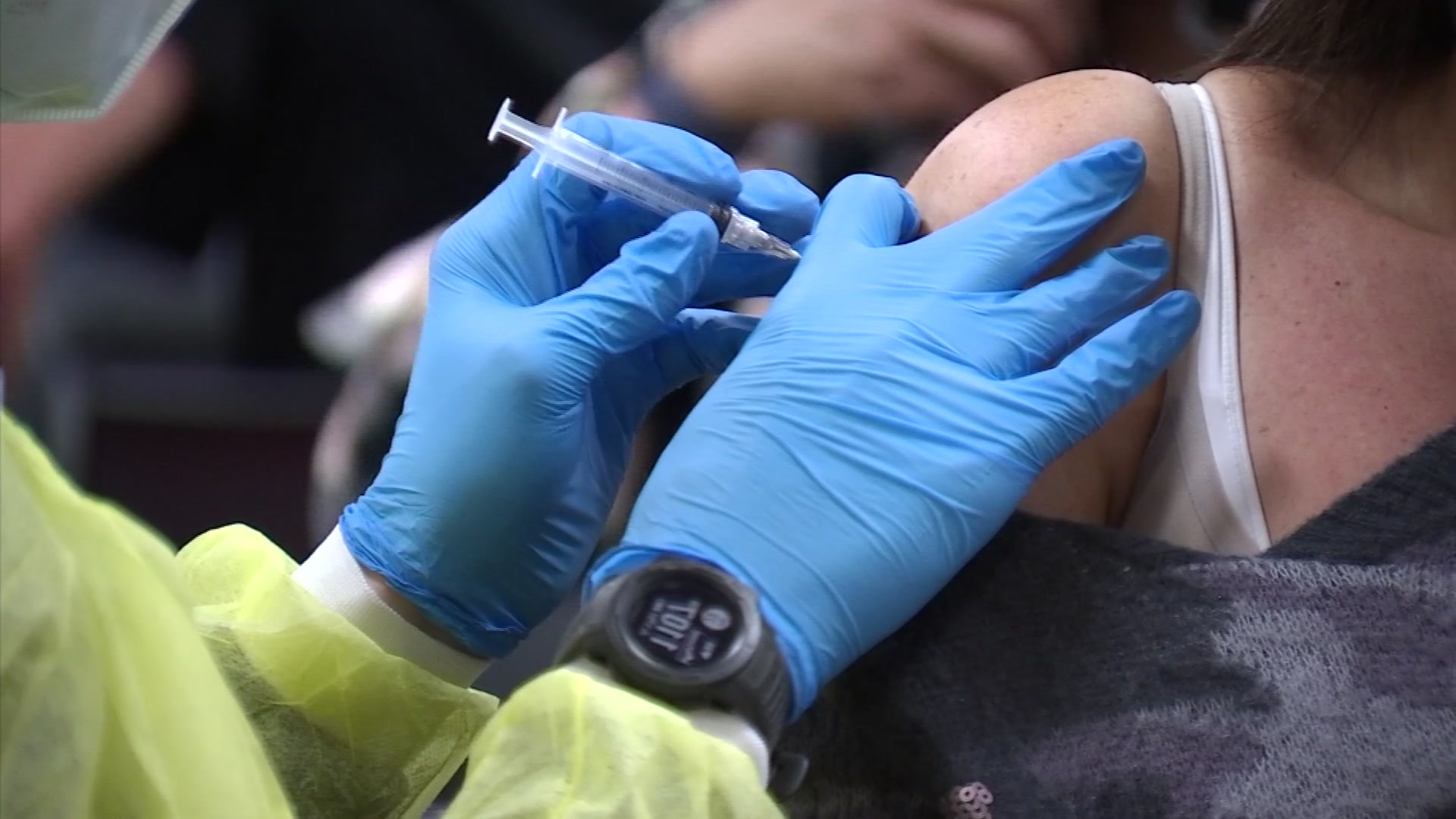
As more and more of the United States population gets vaccinated against COVID-19, many are wondering: when will enough people be vaccinated for life to return to normal? That question doesn't have a simple answer, but scientists are working every day to understand more about herd immunity and how it can help us return to normal life, someday.
Here's what you should know.
What is herd immunity?
Herd immunity, also known as community immunity, is the idea in epidemiology that people can collectively stave off the spread of infections if a certain percentage of the population has immunity to a disease.
Get San Diego local news, weather forecasts, sports and lifestyle stories to your inbox. Sign up for NBC San Diego newsletters.
How does herd immunity work?
Achieving herd immunity means it is unlikely that a disease, in this case COVID-19, can spread from person to person even if a small percentage of the population is not immune.
"Even individuals not vaccinated (such as newborns and those with chronic illnesses) are offered some protection because the disease has little opportunity to spread within the community," the CDC says.
Another way of thinking about herd immunity, according to John Hopkins University Professor of Medicine Dr. Stuart Ray, is to think of it as the point where an outbreak will not kindle into a big epidemic because enough people are protected.
When will the U.S. reach herd immunity?
White House chief medical advisor Dr. Anthony Fauci has previously said that 75% to 85% of the population would need to develop immunity to create an "umbrella" of protection. Officials with the CDC said in January 2021 that upward of 85% of people would need to be covered to achieve so-called herd immunity if a fast-spreading virus variant, such as B117, which was first reported in the U.K., becomes the dominant strain in the U.S.
During a March hearing of the Senate Health, Education, Labor, and Pensions Committee, Fauci stated that the U.S. won't reach herd immunity until children and teens can get COVID-19 vaccines.
"We don't really know what that magical point of herd immunity is, but we do know that if we get the overwhelming population vaccinated, we're going to be in good shape. We ultimately would like to get and have to get children into that mix," Fauci said.
More than half of U.S. adults have gotten at least one COVID-19 vaccine dose, as of April.
The New York Times reported Monday that "there is widespread consensus among scientists and public health experts that the herd immunity threshold is not attainable — at least not in the foreseeable future, and perhaps not ever."
How do people build immunity?
When a person becomes infected, the body naturally wants to fight back. When a person recovers, the immune system "remembers what it learned" about how to protect the body from disease by keeping T-lymphocytes, called memory cells, that can quickly jump into action to fight the disease again, the CDC says.
Vaccines mimic that process, not by infecting an individual, but by causing the immune system to produce T-lymphocytes and antibodies. Vaccines reduce the risk of infection by working with the body's natural defenses to safely develop immunity to the disease.
People can become immune to an infectious disease either through vaccination and/or prior illness, the CDC says.
The two vaccines being utilized in the U.S., Pfizer-BioNTech and Moderna, have shown to be about 95% effective at preventing an individual from getting COVID-19. Studies are being conducted to determine how long a person who is vaccinated will be immune to COVID-19.
There is still more to learn about whether a person with the vaccine or someone who has been infected by COVID-19 can still be a spreader of the virus.
What is waning immunity and how does it work with COVID-19?
Waning immunity is the loss of protective antibodies over time, essentially the length of time after a person is vaccinated or sick with COVID-19 that they loose antibodies and could become reinfected.
The CDC says research is still needed to determine the amount of time people who are vaccinated will have immunity.
There is also limited published research from the CDC about how long a person who was naturally infected by COVID-19 will remain immune. According to a study from the Public Health England published on Jan. 14, 2021, people who were infected with COVID-19 naturally are likely to be protected from reinfection for five months.
Dr. Ray says that it will be important to reassess over time what our level of herd immunity is based on waning immunity.
If I already had COVID-19, do I need the vaccine?
The short answer is: yes. It is rare to be re-infected by COVID-19 but because the CDC does not yet know how long a person who was infected with COVID-19 will stay immune, they suggest getting the vaccine anyway.
But, if you were treated for COVID-19 using monoclonal antibodies or convalescent plasma, you should wait 90 days before getting the COVID-19 vaccine, the CDC says.
Is it better to get immunity from the vaccine or by naturally being infected?
The CDC says natural infections can cause severe complications and be deadly, even for the mildest forms of disease, like chickenpox. "It is impossible to predict who will get serious infections that may lead to hospitalizations," the CDC says.
Vaccines may cause side effects but they are typically mild and won't lead to hospitalization or death. "Even with advances in health care, the diseases that vaccines prevent can still be very serious -- and vaccination is the best way to prevent them," the CDC says.
The simple answer: vaccines do the same thing as catching a disease without actually making you sick.
Why do we need the vaccine? Why don't we let herd immunity occur naturally?
Without a vaccine, it would take much longer to reach herd immunity in the United States and during that time, it would result in many more unnecessary cases and deaths, according to the World Health Organization. The majority of medical professionals support achieving herd immunity through vaccination.
What do the new COVID-19 variants mean for reaching herd immunity?
If the vaccines are able to "evade vaccine-induced immune responses," Dr. Ray says, then they have the ability to hinder our progress to herd immunity, but more research needs to be done on the efficacy of vaccines on different variants. As of now, it doesn't seem likely that the variants will completely evade the vaccine, Ray says.
It is normal that a virus will mutate the more it spreads in a community. It happens every year with the flu forcing scientists to slightly vary flu vaccines in order to prevent spread.
In order to reduce the impact of the variants on our progress towards herd immunity, people should continue wearing masks, social distancing, avoiding indoor gatherings and reducing travel.
"The more people infected, the more chances this virus gets to evolve, because evolution requires diversification, which increases a little every time someone gets infected," Dr. Ray said.
Until we know more about variants and the ability for the vaccine to prevent the spread of COVID-19 from person to person, masks will still be necessary in certain settings. So it may be a while until life returns to "normal."