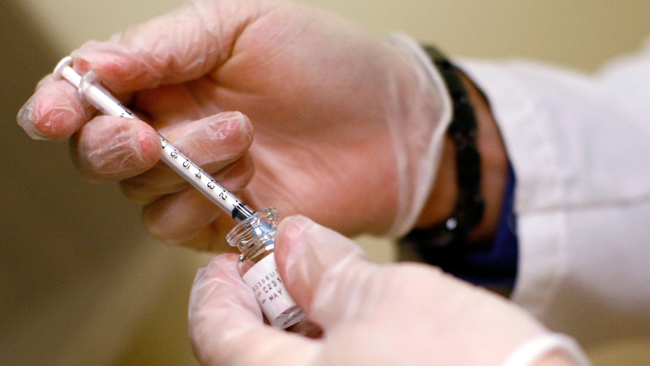
Walk-up COVID-19 testing sites are getting a lot of foot traffic these days, but what if the test comes back positive? And what if that test got it wrong? NBC 7 Investigates learned that it happens a lot more often than you might think.
“I was devastated,” San Diego resident Kim Penny said. “I was horrified. First of all, I’m not sick at all. I had no symptoms.”
Penny described her reaction when she got back her COVID-19 test result last week and read the word "positive."
“The fact that I could have given it to someone else was horrifying to me,” Penny said. “It just -- it was awful.”
Penny canceled her flight and called everyone she had come into contact with. But after catching a discrepancy on the dates on her results, she returned for a second test at a hospital and was told she was, in fact, negative.
“It was so unnecessary and so disrupting to so many people that it was very upsetting,” says Penny.
One of the people Penny contacted was Tony Farwell, a San Diego man who got tested and, like Penny, got a positive result.
Local
“I was certainly surprised,” Farwel said. “I did not expect to get a positive test.”
But after Penny told Farwell she was in fact negative, he took two more tests - both of which also came back negative.
Farwell and Penny are far from alone.
Just last month the FDA put out an alert about false-positive rapid antigen COVID-19 tests. The probability of false-positive tests goes up as the prevalence of the disease goes down.
According to data from the FDA, if an antigen test has 98% specificity, and 10% of the population has the disease, 20 out of 100 people who test positive will not have the virus.
This already seems high but check out what happens if the disease prevalence drops to 1%: 70 out of 100 people who get a positive result, will get a false positive.”
“I do think that’s a wake-up call to the accuracy of these tests,” Farwell said.
Both Farwell and Penny are quick to acknowledge a false negative is far more dangerous than a false positive, but still, Penny believes there should be a better solution.
“Why do we have to have false anything?” Penny said. “The reason we go get tested is to find out if we have COVID-19. And to get a false-either-way is not good. And our science should be at a point where that should just be an unacceptable outcome.”
The pandemic has shown the limits of medical tests, but testing is still the most accurate way to determine who has the virus.
Penny said a false positive doesn’t just take a psychological toll and create a contact-tracing burden; she said she also worries about the impact that false-positives can have on triggering stricter restrictions and shutdowns.
“It is a very strong response to a situation in which we may be dealing with information that is not completely correct,” Penny said.
Bottom line: Both Penny and Farwell said the tests are important, and, along with health professionals, they advise people to get tested if they feel they're at risk. But, consider getting more than one test.
Penny and Farwell took two different types of COVID-19 tests. Penny took a molecular test, and Farwell took a rapid antigen test. While both tests are useful, molecular diagnostic tests are widely considered to be more accurate, although the results take longer to come back.